Conservative and Surgical Foot Care
- Achilles Tendonitis
- Athlete's Foot, Nail Fungus
and Other Nail Conditions - Bunions
- Diabetes
- Flat Feet
- Hammertoes
- Heel Pain
- Neuroma
- Orthotics
- Warts
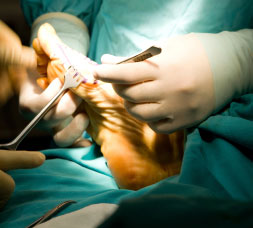
Achilles Tendonitis

The Achilles tendon is the strongest and largest tendon in the body. It attaches the calf muscle (gastrocnemius and soleus muscles) to the heel bone (calcaneus) and is necessary for normal walking, running, and jumping. Athletic and traumatic injuries to the Achilles tendon are common and can be disabling. Achilles tendinitis is an inflammation of the Achilles tendon. The inflammation is most commonly localized to the end of the tendon closest to the heel, and may spread upward to affect even the muscles of the calf. Swelling often occurs and pain can be felt when it contracts. In severe cases, pain may be felt even at rest. Generally, Achilles tendinitis begins as a dull pain at the back of the lower leg just above the heel. Unless the aggravating activity is stopped, the condition can worsen until any activity requiring a push-off from the ground (by the foot) becomes quite painful and nearly impossible. The majority of Achilles tendon injuries are due to overuse. Other factors that lead to Achilles tendonitis are improper shoe selection, inadequate stretching prior to engaging in athletics, a short Achilles tendon, increased pronation of the foot and ankle, direct trauma (injury) to the tendon, training errors and heel bone deformity. Early treatment is advisable (if not absolutely necessary) to avoid potential tear or rupture.
Athlete's Foot, Nail Fungus and Other Nail Conditions
Because of the environment our feet find themselves daily, Athlete's Foot (tinea pedis) is a common skin concern. Caused by a fungal infection, it usually occurs between the toes. The fungus thrives on our feet because of the warm, dark, and humid environment in our shoes, which encourages the fungus to grow. Symptoms of Athlete's Foot include dry, scaling skin, with cracking and peeling. It can be inflamed and show blisters on and between the toes. It may also spread to the soles of the feet, as well as other parts of the body. When there is excessive overgrowth on the feet, this can lead to fungal infection of the nails (onychomycosis); this is why timely treatment is very important.
Whenever there is a crack or break in the nail plate, this gives access to the nail bed. Once the fungus invades this area, it multiplies slowly over time, using the nail as protection from being removed with normal bathing. A fungal infection can affect one nail, or, if the conditions are right, affect all nails at the same time. The infection can cause destruction of nail and create debris that forces the nail upward, discoloring it in the process. The nail thickens, become crumbly, and become generally misshapen. Some nails may fall off completely.
Ingrown toenails, particularly on the sides of the big toes, are usually caused by trimming toenails too short. Additionally, shoe pressure, injury, heredity, and poor foot structure can cause problems. Often causing pain, ingrown toenails occur when the corners or sides of the toenail dig into the skin. Left untreated, they may become sore, reddened, and infected. Other nail conditions include black or darkened toenails, essentially bruising of the nails from multiple small injuries. This may occur as a result of the toe hitting the end or top of the shoe toebox.
Many nail conditions are difficult to treat on your own, and medication may necessary whether topical or oral. We can help in making the best decision for your condition.
Bunions
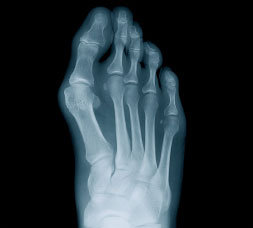
Our great toe provides leverage and balance when we walk, and works exceptionally hard supporting our weight. Changes in position of the toe or enlargement of bone at the joint can cause pain, and is typically referred to as a bunion. There are two main types of bunions-acquired and structural.
Acquired bunions can be caused by excess pressure, injuries and arthritis. These factors cause extra bone to form and joint tissues to thicken, enlarging the site over time. Structural bunions are based on your genetics. The structure of your foot, in most part, is inherited. These bunions may be noticed at an early age (juvenile bunion), and relate to both joint position and general bone growth.
Overall, the vast majority of bunion deformities have a structural component allowing the acquired causes to become painful. Shoes, activities and foot structure all play roles in how a bunion is evaluated. It can help with the decision making process. If simple changes in shoe gear or activities do not relieve symptoms, the foot structure needs to be evaluated. This can be through biomechanical changes, such as orthotics, splinting or surgically reducing the bunion and aligning the great toe. If surgery is indicated, understand that there is no one bunion correction which fits everyone. Individual factors (health, foot structure and activities) will play a role in choosing the right procedure.
Diabetes
With diabetes, there are increased health risks even with minor foot problems. Reduced sensation (neuropathy) and restricted blood flow (PAD) make detecting tissue injuries on the feet, and healing that tissue, difficult. It’s important to maintain a consistent foot health program, including visits to a podiatrist to discuss and evaluate the condition of your feet. Circulation, skin and bone problems can be identified in your exam based on color changes, swelling, temperature and sensation changes, pressure points, cracks or ulcers, and nail condition. We will discuss proper homecare, including self-foot inspection and understanding the warning signs of infection. If you think a problem is at hand, contact us for an evaluation. In the course of managing your diabetes with your primary care physician, periodic foot care evaluations will help maintain an overall healthy lifestyle for you and your feet.
Flat Feet
There are many different causes and types of flat feet. Congenital flat foot is a condition that one is born with. This foot type is a result of the fact that all people are born with different features. In other words, it’s in your genes. This foot structure type may or may not cause problems later in life. Acquired flat foot, which develops over time, is more likely to cause pain and other symptoms – including the development of arthritic joints, chronic tendonitis and plantar fasciitis. Many different factors can contribute to the development of flat feet. These include a child's sitting or sleeping positions, compensation for other abnormalities further up the leg (length differences), or more severe factors such as rupture of ligaments or tendons in the foot. A common cause for flat feet is that the foot is compensating for a tight Achilles tendon. If the Achilles tendon is tight, then it causes the foot flatten. The most common acquired flat foot in adults is due to Posterior Tibial Tendon Dysfunction (PTTD). The posterior tibial tendon is the tendon that helps support the arch, which over time can stretch and lose its tension. Flat feet can be addressed both conservatively and surgically.
Hammertoes

The small toes on our feet bend to grip the ground, helping with our sense of balance. Sometimes the muscles and joints can change over time, causing the toe to “kink-up” or “curl under”. These are called hammertoes. They are caused when there is a muscle imbalance or a structural abnormality (heredity). They may be acquired overtime or noticed early in life, part of an inherited foot structure. Regardless if they are acquired or inherited, hammertoes may become painful based on shoe choices, activities or injuries. We can help with the decision making process on how to address your discomfort. If simple changes in shoe gear, activities or splinting the toe do not relieve symptoms, it may need to be corrected surgically. If surgery is indicated, individual factors will play a role in choosing the right procedure.
Heel Pain
There are number of causes for heel pain, the most common being stress on the plantar fascia. This is the ligament that runs from the ball of the foot to the heel, supporting the arch. The condition is known as plantar fasciitis. An excessively flat foot or a shortened/very tight plantar ligament can cause strain on the fascia, leading to pain and discomfort. Symptoms are commonly noticed on the first steps in the morning and when attempting to walk after a period of sitting. It may also be noticed after long periods of standing or strenuous activity. A heel spur can be found secondary to long-standing plantar fasciitis. This is the body attempting to repair where the plantar fascia pulls away from the heel. Minor symptoms can be relieved by stretching, acupressure and ice/heat therapy. Also, choosing the correct shoe for the activity, and using a quality pre-fabricated or custom orthotic can help with long-term relief. If symptoms persist, surgery may be necessary.
Neuroma
A neuroma is an enlarged, irritated nerve caused when the bones of the forefoot compress upon it. This may be due to abnormal bone structure and from excess pressure caused by specific shoes and/or activities. It is most commonly found between the 2nd and 3rd or 3rd and 4th toes. This is usually felt as a sharp sensation in the ball of the foot, radiating to the toes with pain and/or numbness. Treatment can include injections, shoe gear alterations, orthotics and possible surgery.
Orthotics
Custom orthotics are specialized shoe inserts, molded specifically for you from an impression of your foot. These can help improve overall function of the feet. Many biomechanical conditions can benefit from orthotics, and they are most effective when worn in all shoes possible. Along with the foot, orthotics can help with ankle, knee, hip and back problems by aligning joints from the bottom up. Just as no two feet are alike, there is no one orthotic that fits all (“custom” orthotics can’t be found at your local drug store). Foot structure, activity level and shoe types all play a role in constructing the correct orthotic for you. To obtain the best results, and since they will work your muscles differently, some time may be needed to break them in.
Warts
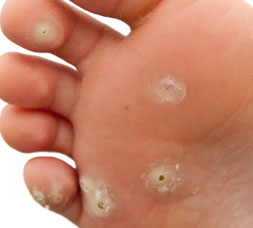
Warts are a virus that your body has “accepted” as not being a problem. They most commonly occur on contact areas such as the feet and hands. They are contagious and can spread to other locations, and other people, through breaks in the skin. Warts can be painful, unsightly, and also recurrent. Many over-the-counter treatments take a long time to work, if effective at all. Additionally, there are other skin conditions which appear similar to warts, are painful and resistant to home treatments. We can identify the differences, and discuss topical and surgical options available through our office for a more efficient result.











